Antibiotic Resistance: Onions to the Rescue
More Information
By Dr. Mercola
As a close relative to onions, shallots provide some of the same benefits, including anticancer, anti-inflammatory and antioxidant properties. Now, researchers have determined certain antibacterial molecules from the Persian shallot, a staple of Iranian cooking, have the potential to combat multidrug-resistant tuberculosis (MDR-TB).1
If you suffer from a bacterial infection, you will very likely be prescribed an antibiotic. In the case of TB, you will very likely be prescribed not one, but a cocktail of four antibiotics, including isoniazid and rifampicin. Due to numerous factors, including overuse and poor gut health, antibiotics are becoming less effective because bacterial pathogens continue to develop drug resistance.
Given the fact MDR-TB infected nearly half a million people in 2016, killing more than 78,000,2 drug-resistant TB is a significant concern. Using shallot extract to boost the effectiveness of existing TB-related antibiotic treatment has the potential to save many lives.
Shallots May Be Useful to Help Combat Antibiotic Resistance
While you may enjoy cooking with shallots, which possess many of the same health benefits as onions, researchers at University College London and Birkbeck, University of London, are exploring their potential to fight forms of drug-resistant TB.3 It appears the antibacterial properties extracted from the Persian shallot may be useful to increase the effectiveness of existing antibiotic treatment. The particular shallot species in question is Allium stipitatum, which is native to central and southwestern Asia.4
After synthesizing various compounds found in the Persian shallot to enhance its antibacterial properties, researchers tested the compounds on several types of drug-resistant bacteria. One of the types tested was Mycobacterium tuberculosis, the bacterial species known to cause TB. The shallot compounds were found to have inhibitory effects against:5,6
- Escherichia coli (E. coli): Large, diverse group of bacteria found in the environment, food and intestines of animals and people; while most strains of E. coli are harmless, others can cause diarrhea, pneumonia, respiratory illness and urinary tract infections
- Klebsiella pneumoniae: Can cause health care-associated infections such as meningitis, pneumonia and surgical-site or wound infections
- MDR Staphylococcus aureus: Genetically different from other strains of Staphylococcus aureus and responsible for several difficult-to-treat conditions such as sepsis (blood poisoning) and skin infections
- Proteus mirabilis: A pathogen frequently found in the urinary tract, particularly in patients undergoing long-term catheterization
One molecule in particular, deemed to be the most promising, inhibited growth of isolated Mycobacterium tuberculosis cells by more than 99.9 percent.7 Although the research is ongoing and clinical trials would be needed to affirm the efficacy of these chemical compounds for medical treatment, the four shallot molecules tested to date significantly reduced bacteria in MDR-TB.
About the results, study author Sanjib Bhakta, Ph.D., head of Birkbeck, University of London’s Institute of Structural and Molecular Biology Mycobacteria research lab, said:8,9
“Despite a concerted global effort to prevent the spread of tuberculosis, approximately 10 million new cases and 2 million deaths were reported in 2016. As many as 50 million people worldwide are currently infected with MDR-TB, which means it’s vital to develop new antibacterials.
In searching for new antibacterials, we tend to focus on molecules that are potent enough to be developed commercially as new drug entities by themselves. However, in this study we show that by inhibiting the key intrinsic resistance properties of the TB, one could increase the effects of existing antibiotic treatment and reverse the tide of already existing drug resistance.”
Should the shallot research continue to advance, scientists hope to one day pair these promising plant compounds with antibiotics already being used to combat strains of TB that have developed resistance to antibacterial drugs.
Professor Simon Gibbons, study author and head of University College London’s department of pharmaceutical and biological chemistry, stated, “Natural products from plants and microbes have enormous potential as a source of new antibiotics. Nature is an amazingly creative chemist … We believe nature holds the key for new antibiotic chemotypes.”10
What Causes Antibiotic Resistance?
According to the U.S. Centers for Disease Control and Prevention (CDC),11 drug resistance happens within the context of fighting germs. Some germs are drug resistant. Antibiotics kill not only the bad bacteria causing your illness, but also your good gut bacteria — the ones that help protect your body from infection.
With less good bacteria to fight back, the drug-resistant bacteria are able to grow and take over. Even worse, some of the bad bacteria pass along their drug-resistance abilities to other bacteria, exacerbating the problem.
This is, in part, why it is important to replenish your gut bacteria after completing a course of antibiotics. You need to rebalance your gut flora. Using even a single round of antibiotics, therefore, contributes to the development of drug resistance. For this reason, antibiotic drugs should only be used to treat bacterial infections — for example, pneumonia, strep throat and urinary tract infections.
It’s important to note antibiotics have zero effect on viral infections, such as the common cold or flu. Your body recovers from viral infections only after the illness has run its course. Taking antibiotics for viral infections is unnecessary and dangerous since it contributes to the problem of drug resistance. About antibiotics, the CDC says:12
“Antibiotics are among the most commonly prescribed drugs used in human medicine, and can be lifesaving drugs. However, up to 50 percent of the time, antibiotics are not optimally prescribed, often done so when not needed [and given with] incorrect dosing or duration.”
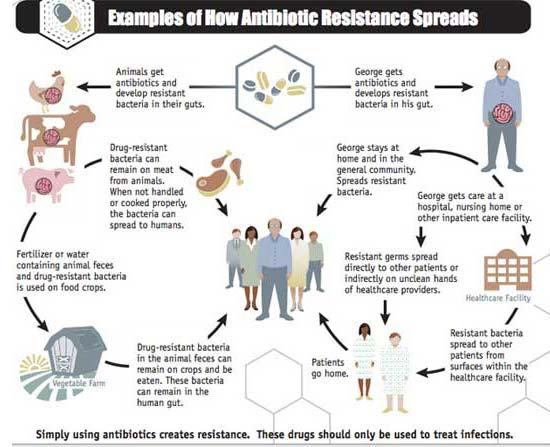
As shown in the diagram below, other major factors in the growth of antibiotic-resistance is the spread of resistant strains of bacteria from person to person or from animals to people through the food supply.
Beyond the human misuse of antibiotics, the pervasive abuse of these drugs by the agriculture industry also plays a significant role, accounting for about 80 percent of all antibiotics used in the U.S. Concentrated animal feeding operations (CAFOs), in particular, are hotbeds for breeding antibiotic-resistant bacteria because CAFO animals are routinely fed continuous low doses of antibiotics, which enables pathogens to survive, adapt and eventually thrive.
Source: CDC.gov, Examples of How Antibiotic Resistance Spreads, 2013
How Big of an Issue Is Antibiotic Resistance?
Simply stated, drug resistance results when infection-causing bacteria, fungi, parasites or viruses evolve and become immune to a drug that was once able to destroy them. Instances of drug resistance continue to rise, with about 2 million drug-resistant infections occurring annually in the U.S., resulting in the deaths of an estimated 23,000 people each year.13 According to BBC News,14 25,000 people across Europe die each year from drug-resistant infections. TB-related drug resistance takes multiple forms, including:15
- Mono-resistance: characterized by resistance to one first-line anti-TB drug only
- Poly-resistance: involves resistance to two or more first-line anti-TB drugs, other than isoniazid and rifampicin
- MDR: notable by resistance to at least both isoniazid and rifampicin
- Extensive drug resistance (XDR): distinguished by resistance to any fluoroquinolone, and at least one of three second-line injectable drugs — amikacin, capreomycin and kanamycin — in addition to MDR
- Rifampicin resistance (RR): features resistance to rifampicin, with or without resistance to other anti-TB drugs, including RR in the form of mono-resistance, poly-resistance, MDR or XDR
About MDR-TB the World Health Organization says:16
“Anti-TB drug resistance is a major public health problem that threatens progress made in TB care and control worldwide. Drug resistance arises due to improper use of antibiotics in chemotherapy of drug-susceptible TB patients. This improper use is a result of a number of actions including, administration of improper treatment regimens and failure to ensure patients complete the whole course of treatment.
Essentially, drug resistance arises in areas with weak TB control programs. A patient who develops active disease with a drug-resistant TB strain can transmit this form of TB to other individuals.”
Lifestyle Factors That Can Help You Avoid Antibiotic-Resistant Disease
You can help yourself and the community around you by purchasing only antibiotic-free grass fed meats and taking oral antibiotics only when absolutely necessary. While the problem of antibiotic resistance is an issue requiring global resolution, the potential impact on you personally is significant.
Your lifestyle choices are the most critical factors in determining the health of your immune system, and the strength of your immune system influences your ability to resist infections. Below are some basic strategies for supercharging your immune system. In addition, you may want to download my report about how to protect yourself from super germs.
• Optimize your diet. Avoid foods known to tax your immune system, such as grains, processed foods and sugar. Reduce your net carbohydrates (fructose, grains and sugar), moderate your protein intake and increase your healthy fat intake — saturated and monounsaturated fats from animal and tropical oil sources.
Most of your diet should be fresh, whole foods, like organic vegetables, grass fed dairy and meats and beneficial fats such as avocados, coconut oil, grass fed butter and olive oil (used cold). Seventy to 80 percent of your immune system resides in your gastrointestinal tract, and it depends on a healthy, balanced gut flora. One of the best ways to support your gut microbiome is by regularly eating fermented foods.
• Exercise regularly. Exercise improves the circulation of immune cells in your blood. The more effectively these cells circulate, the more efficient your immune system will be at locating and eliminating pathogens. Make sure your fitness plan includes core work, high-intensity exercise, stretching and weight training.
• Get plenty of restorative sleep. Research shows sleep deprivation has the same effect on your immune system as physical stress or disease, which is why you may feel ill after a particularly poor night of sleep. The average adult requires seven to nine hours of sleep a night.
• Be proactive in addressing stress. High levels of stress hormones can diminish your immunity, so be sure you have some sort of stress management program in place. Meditation, prayer, yoga and the Emotional Freedom Techniques (EFT) are all excellent strategies for managing stress; take time to find what works best for you.
• Optimize your vitamin D levels. Studies have shown inadequate vitamin D can increase your risk for methicillin-resistant Staphylococcus aureus (MRSA) and other infections, which can likely extend to other superbugs. Sensible sun exposure at or around midday is your best source of vitamin D.
If you live in a northern climate and cannot get regular sun exposure, consider taking an oral vitamin D3 supplement along with vitamin K2 and magnesium. Be sure to check your levels at least twice a year to ensure they’re in the therapeutic range — 60 to 80 nanograms per milliliter seems to be the ideal range.
Natural Agents Known to Possess Outstanding Antibacterial Properties
In addition to the lifestyle measures listed above, several natural agents have been shown to possess outstanding antibacterial properties, including:
|
Colloidal silver Colloidal silver has been regarded as an effective natural antibiotic for centuries, and research shows it can even help eradicate antibiotic-resistant pathogens. If you are interested in this treatment, make sure you follow the guidelines for safe usage of colloidal silver due to the risks associated with improper usage. |
|
Copper fixtures Replacing fixtures in hospitals and nursing homes with certain copper alloys can help kill bacteria, even superbugs. Installing copper faucets, light switches, push plates and toilet seats in germ-infested areas could potentially save thousands of lives each year.17,18 |
|
Garlic Garlic is a powerful antibacterial, antifungal and antiviral known to stimulate your immune system, assist wound healing and kill antibiotic-resistant bacteria, including MRSA and MDR-TB. For the maximum potency, eat garlic fresh and raw — chopped or smashed. |
|
Manuka honey Manuka honey, made from the flowers and pollen of the Manuka bush, has been shown to be more effective than antibiotics in the treatment of serious, hard-to-heal skin infections. It inhibits bacteria responsible for wound infections, including superbugs such as MRSA that are resistant to multiple antibiotics.19 |
|
Olive leaf extract In vitro studies show olive leaf extract is effective against Klebsiella, a gram-negative bacterium, inhibiting its replication, in addition to being toxic to other pathogenic microbes.20 |
|
Tea tree oil Tea tree oil is a natural antiseptic proven to kill many bacterial strains, including MRSA.21 |
|
Vitamin C Vitamin C’s role in preventing and treating infectious disease is well established. Intravenous vitamin C is an option, but if you don’t have access to a practitioner who can administer it, liposomal vitamin C is the most potent oral form. For more information on vitamin C, listen to my interview below with Dr. Ronald Hunninghake, an internationally recognized vitamin C expert. |
Source:: Mercola Health Articles


 Body Charge Nutrition is a premium nutritional supplement provider based in Western Canada offering only products and information that are of the highest quality and integrity. Through knowledge and personal experience, it is our goal to assist you with taking control of your health.
Body Charge Nutrition is a premium nutritional supplement provider based in Western Canada offering only products and information that are of the highest quality and integrity. Through knowledge and personal experience, it is our goal to assist you with taking control of your health.